UNDERSTANDING MENTAL ILLNESS AND CHRONIC PAIN
WHAT IS ACUTE PAIN AND HOW IS IT DIFFERENT FROM CHRONIC PAIN?
Acute pain is the pain you would experience following a new injury. So, this could be a bone fracture, a muscle strain or a soft tissue damage such as a cut. The pain can last as little as a few moments or up to 3-6 months. Thus, body’s pain system is responding appropriately to the related injury.
However, for chronic pain, the pain is still real, but it is not due to a new injury or harm. The pain may not be associated with an actual injury and persists beyond the normal healing time which is between 3-6 months.
The pain is prolonged, the body’s pain system is altered, and it no longer represents an injury. Common types of chronic pain may include back pain, neck pain, cancer pain, headaches or migraines.
THE FIRE ALARM
Pain is like a fire alarm. It is there to protect you. Like a fire alarm that alerts people of threat to fire, the pain system similarly is an internal alarm system that alerts your body that there is a threat of damage to your body.
However, in chronic pain, the fire alarm is no longer functioning effectively, and it continues to go off even after the fire is being put out.
The fire alarm has become more sensitive and may go off at any time. In other words, in chronic pain, your pain system is giving you pain signals despite no injury.
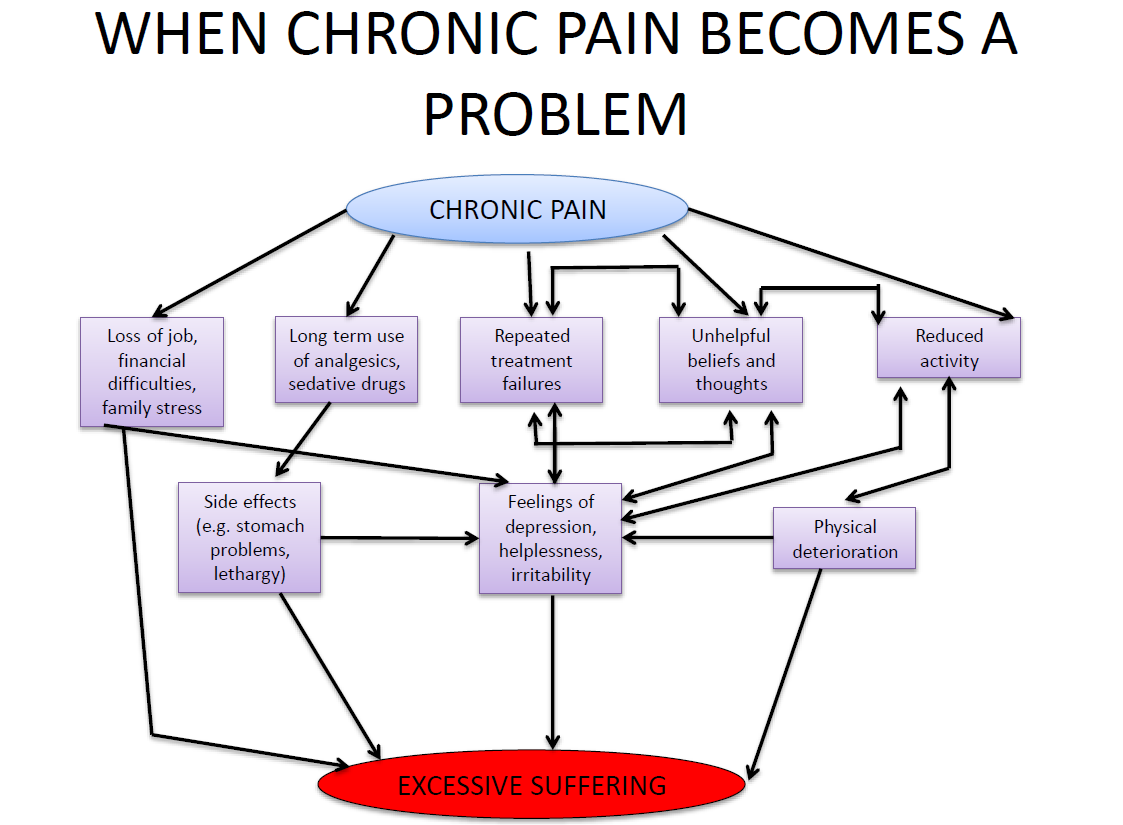
Extracted from:
Nicholas M, Molloy A, Tonkin L., Beeston L. Manage your pain: Practical and Positive ways of Adapting to Chronic Pain. Souvenir Press. 2011.
Chronic pain is a feeling of prolonged and persistent pain over time. Having to experience such pain for a long duration will impact several areas of a person’s life.
Having chronic pain may have led a person to lose jobs, experience financial difficulties and having ongoing family conflict and stress.
In order to manage pain, a person may also be ‘hooked’ to several use of pain killers for a long duration of time. Some may go from one doctor to another doctor, looking for “the cure” to the pain.
Due to the pain, a person starts to be inactive, or no longer engaging in things that they enjoy or use to do. When a person is no longer able to function as best as they could, they may start to have more unhelpful thoughts.
It may include thoughts such as “I’m not good enough” or “I can’t do anything now” or “nobody cares” in which can lead to feelings of despair, depression, helplessness, frustration and irritability. Thus, despite starting off as a physical pain, chronic pain causes significant impact on almost every aspect of a person’s life including social, occupational and financial and of course mental health.
As this cycle continues, it creates an even bigger impact on the person’s overall life and wellbeing. This in which causes excessive suffering for the individual.
CHRONIC PAIN AND MENTAL HEALTH
Chronic pain is interconnected with depression, anxiety, and negative beliefs about pain. These mental health issues are all related to not only developing chronic pain but also the worsening outcomes due to chronic pain.
- 20–50% of patients with chronic pain have co-morbid depression,
- patients with severe pain are more likely to be depressed.
- There is a bidirectional relationship between mental illness and chronic pain meaning
- Chronic pain can cause poor mental health
- Poor mental health can cause chronic pain
- Anxiety and fear about pain are linked to a higher likelihood of developing chronic pain
- Anxiety and fear are linked to poorer prognosis of recovery from chronic pain
Managing chronic pain, cannot be treated as just physical pain and in silo. It impacts a person’s overall wellbeing. Therefore, managing chronic pain needs to be addressed holistically. What has been found useful is a multidisciplinary approach to managing chronic pain with the help of a pain specialist, a psychologist and a physiotherapist.
As finding a cure may be something that many have tried, as frustrating as it is, a person struggling with chronic pain may start to realise that there is no specific cure. There may be some treatment that provides short-term relief, but has not been lasting or providing “the cure they need”.
One thing for sure, as the journey to find a “a cure” continues, it takes them away from enjoying life and being the person, they want to be in which inevitably impacts on their wellbeing.
Thus, unlike acute pain where you need the rest to heal, managing chronic pain is about learning ways to manage the pain and continue living and enjoying life. As uncomfortable as it is to hear this, shifting the thoughts of finding a cure towards realising that the pain may not go away, but to manage the pain better so that you can still do what you enjoy in life is the way forward.
Seeing a psychologist can help in managing the anxiety, frustration and depression that comes along in managing chronic pain. Managing these difficult emotions is important, as if it was left unattended, untreated or even “dismissed”, it would further cause greater pain, poorer prognosis and a barrier towards effective management.
Psychologist can further help identify and work towards achieving SMART goals, identify unhelpful thoughts and behaviour that may contribute towards the cycle of “excessive suffering”, building skills and strategies for pain management, aimed towards living a rich and meaningful life.
All in all, chronic pain is not just physical, it impacts a person’s overall well-being, including occupational, financial, social and emotional being. Managing chronic pain needs to be approached holistically.
Mental health associated with chronic pain further exacerbates the pain causing excessive suffering. Thus, it is important to reach out and seek help as managing chronic pain should not be done alone.
Reference:
Mills SEE, Nicolson KP, Smith BH. Chronic pain: a review of its epidemiology and associated factors in population-based studies. Br J Anaesth. 2019 Aug;123(2):e273-e283. doi: 10.1016/j.bja.2019.03.023. Epub 2019 May 10. PMID: 31079836; PMCID: PMC6676152.
Nicholas M, Molloy A, Tonkin L., Beeston L. Manage your pain: Practical and Positive ways of Adapting to Chronic Pain. Souvenir Press. 2011.
About Author:
Dr Aida Suhaimi is a DHA licensed Clinical Psychologist with over 10 years of experience in the field. Dr Aida loves her work as a clinical psychologist and passionate about supporting people to reach their full potential. She works with children, adolescents and adults. Her training and clinical experience have been within the settings of community mental health clinics, schools, hospitals and mental health institution.
Dr Aida Suhaimi provides psychological assessments for both children and adult population. Dr Aida conducts psychoeducational assessments (including IQ testing, achievement abilities, emotional and behavioural difficulties, adaptive functioning), neuropsychological assessments (including cognitive abilities, executive functioning, memory) and personality testing.
Dr Aida Suhaimi provides psychotherapy and uses evidence-based practice to support individuals with a range of disorders from depression, anxiety, OCD, panic, specific phobia, depression, post-natal depression, stress, adjustment disorder, low self-worth and other emotional and behavioural difficulties.
Acknowledging each person’s unique struggles and appreciating each person for who they are, she tailors her treatment to best suit their strengths and vulnerabilities. She incorporates evidence-based approaches with her main areas of expertise include but not limited to Acceptance Commitment Therapy (ACT), Cognitive Behavioural Therapy (CBT), Mindfulness and person-centered approach.
Author
Dr Aida Suhaimi
- Clinical Psychologist





